Scientific Center of Family Health Problems and Human Reproduction, Irkutsk, Russia
High alcohol consumption is a social problem in our country and the world. The paper analyzes Russian and foreign literary sources for studying fetal alcohol syndrome (FAS) and fetal alcohol spectrum disorders (FASDs). By now, there have been a certain amount of studies on female alcohol use during pregnancy. FAS is observed for 1000 live newborns. There is no standard accounting system for the diagnosis of FAS/FASDs in any country of the world. A historical reference is given regarding the nature of alcohol effect on the fetus; however, the problem of the effects of alcohol metabolites at the biochemical and molecular levels requires further investigation. The babies who were born with the signs of FAS are noted to have phenotypic changes in the cerebral cranium and viscerocranium, morphological changes in brain tissue, mental disorders, and behavioral, neurological disorders. To prevent the occurrence of FAS/FASDs in children, it is necessary to enhance the role of medical workers in educating young people about the risk factors of these diseases.
Conclusion: the dissemination of modern information and the transfer of knowledge to pregnant women and reproductive-aged women by physicians, psychologists, social pedagog-ists, and social workers about the irreparable harm of their alcohol use done to the child are extremely important to prevent FAS and FASDs.
It is necessary to fix the attention of the society on the problem of FAS, to popularize a healthy lifestyle, to foster the alcohol use culture, as the ubiquitous availability of alcoholic beverages and the lack of self-discipline lead to harmful consequences.
Authors' contributions: Marianian A.Yu., Rychkova L.V. – the concept and design of the investigation, editing and approving the publication; Anismova A.O., Rashidova M.A., Kalkova A.N., Muradyan A.E. – material collection and processing, literature search for Russian and international studies in the Russian and international databases; Anisimova A.O., Kalkova A.N., Muradyan A.E. – analyzing the data of the published studies, writing the text.
Conflicts of interest: The authors declare that there are no conflicts of interest.
Funding: The authors declare that there is no external financing to conduct the investigation and to publish the article.
For citation: Marianian A.Yu., Anisimova A.O., Kalkova A.N., Rashidova M.A., Rychkova L.V., Muradyan A.E. Long-term consequences of the effect of alcohol on the fetus.
Akusherstvo i Ginekologiya/Obstetrics and Gynecology. 2023; (6): 16-22 (in Russian)
https://dx.doi.org/10.18565/aig.2022.276
pregnancy
fetus
alcohol
fetal alcoholic syndrome
fetal alcohol spectrum disorders
Токсическое воздействие этанола на плод
Высокое потребление как слабого, так и крепкого алкоголя является социальной проблемой России и представляет серьезную угрозу демографии страны [1, 2]. За последние три года (2020–2022) во время пандемийного кризиса в России заметно выросло потребление спиртных напитков, хотя, по данным ВОЗ, среднее потребление алкоголя в России ниже уровня таких стран, как Германия, Франция и Испания. Алкоголь вызывает различные заболевания, отрицательно влияет на психическое здоровье и здоровье женщин репродуктивного возраста, так как негативно воздействует на развитие плода в период беременности [3–5].
Ученые при анкетировании женщин детородного возраста России и других стран выявили, что большинство из них употребляли алкоголь до беременности и во время беременности [6–8], полагая, что небольшие дозы алкоголя не навредят плоду.
В 1967 г. французские исследователи под руководством врача Lemoine P. впервые научно описали нарушения у детей [9], рожденных женщинами, употребляющими алкоголь во время беременности; в 1973 г. ученый Jones K.L. дал название таким нарушениям – «фетальный алкогольный синдром» (ФАС) [10]. Еще в XVIII в. врачи, общественные деятели начали говорить о пагубном воздействии на плод алкоголя. Эта тема прослеживается в произведениях литературы, живописи, в религиозных источниках; в православной традиции жениху и невесте запрещено употреблять алкоголь на свадьбе; в странах Востока у мусульман по настоящее время существуют строгие законы в отношении алкоголя [11].
До 1970-х гг. прошлого столетия при угрозе преждевременных родов осуществляли внутривенное введение алкоголя [12].
В настоящей работе проанализированы результаты российских и зарубежных литературных источников по изучению ФАС, данные по отдаленным последствиям употребления алкоголя беременными женщинами, а также исторические и современные представления о ведении пациентов, подвергшихся внутриутробному воздействию алкоголя.
ФАС – это комплекс отклонений у новорожденных, которые возникают из-за воздействия спиртного, употребляемого женщиной до и во время беременности, и остаются у ребенка на всю жизнь [13]. Фетальный алкогольный спектр нарушений (ФАСН) – это общий термин, описывающий врожденные дефекты детей, пострадавших от пренатального воздействия алкоголя. Последствия проявляются нарушениями нервной системы, умственной, физической неполноценностью, а в дальнейшем – трудностями с письмом, рисованием и при взаимодействии с окружающими.
По МКБ-10 ФАС относят к XVII классу: Поражения плода и новорожденного, обусловленные употреблением алкоголя матерью: пороки развития, врожденные аномалии, хромосомные нарушения и деформации и т.д. Код Q86.0 [13].
Токсическое воздействие этанола зависит от количества алкоголя и продолжительности его употребления [14]. Объем этанола определяется в дозах. Стандартные дозы выражаются в граммах этанола и различаются по странам, например, в Австралии и Франции – 10 г; в Мексике – 13 г; в Великобритании – 8 г; в Аргентине и Чили – 14 г; в России – 10 г (что соответствует 250 мл пива, 100 мл вина (12%), 30 мл крепкого алкоголя (40%)).
Некоторые ученые полагают, что критическим количеством этилового спирта для возникновения ФАС у новорожденных могут стать 30 г в сутки, однако большинство авторов утверждают, что не существует даже минимальной безопасной дозы алкоголя [15, 16].
Для постановки диагноза ФАС/ФАСН выявляют определенные клинические признаки, указанные в зарубежных системах (отечественных разработок нет): IОМ (руководство института медицины для ФАС, 1996) [17]; четырехцифровой диагностический код Вашингтонского университета, 1997 (обновлен в 1999 г. и в 2004 г.) [18]; CDC (Центр по контролю и профилактике заболеваний, 2004, США) [19]; Hoyme (2005 [20]; разработана для дополнения IОМ) и канадские рекомендации по диагностике FASD (2005) [21]. CDC играет большую роль в мире в изучении и профилактике патологии новорожденных. Рекомендации CDC основаны на реальных исследованиях ученых, клинической экспертизе и опросах семей о проявлении ФАС.
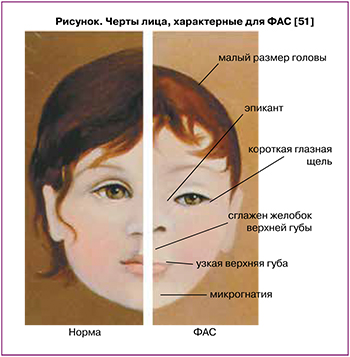
Для подтверждения диагноза ФАС необходим положительный результат по следующим критериям [22, 23]: недостаток пренатального или послеродового роста и (или) массы тела; челюстно-лицевые (рисунок) аномалии (маленькие глазные щели, одно или оба глазных яблока уменьшены в размере, сглаженная бороздка между носом и верхней губой, истонченная верхняя губа, неразвитые верхняя или нижняя челюсти, глубокие ушные раковины, короткий нос, монголоидный разрез глаз); поражения со стороны центральной нервной системы (череп меньше, чем у здоровых младенцев, полное или частичное отсутствие мозолистого тела, мозг недоразвит, нарушения мелкой моторики, врожденное снижение слуха и т.д.); дородовое воздействие алкоголя (неизвестное или подтвержденное беременной женщиной).
Эпидемиология фетального алкогольного синдрома
ФАС отмечается на 1000 живых новорожденных в мире в среднем в 1–1,5 случаях, и этот показатель изменяется в разных странах. Например, в Европе, по данным 2005 г., – 0,97; в США – 0,2–2 случая на 1000 новорожденных [24]. ФАСН, по данным 2001–2004 гг., выявляется чаще: 10 на 1000 живорожденных.
В Италии при обследовании младших школьников уровень заболеваемости ФАС – 4,0–12,0 случая на 1000 человек; частичный ФАС – 18,1–46,3 на 1000 детей [25].
В Великобритании нет систематического отслеживания. Примерная частота случаев ФАС в Англии и Шотландии – 0,21 на 1000, а у детей младше 15 лет, по данным в рамках проекта медицинской специализации, – 0,8 на 1000.
Во Франции национальные исследования проводились каждые 3 года. По данным Бюллетеня института медицинского контроля за 2006–2007 гг. частота ФАС по городам: Эльзас в 2007 г. – 0,29 случая на 1000; Рона в 2007 г. – 0 случаев; Париж в 2006 г. – 0,42 случая на 1000; Изер, Париж, Овернь в 2007 г. – ни одного случая. Продолжения таких исследований нет.
В США не существует долгосрочной системы контроля и учета, и точные цифры по ФАС неизвестны. Примерное количество – от 3,0 до 5,6 случая на 1000 человек; ФАСН – 10 случаев на 1000.
В Западной Австралии ФАС зарегистрирован в 0,02 случаях на 1000 новорожденных для некоренных австралийцев и в 2,76 случаях на 1000 рождений – для коренных. Только 12% австралийских специалистов здравоохранения имеют представление о диагностике и симптоматике ФАСН.
Наибольшее количество ФАС зафиксировано у детей Южной Африки – 40,5–46,4 на 1000 детей; самое низкое в Японии – менее 0,1 на 1000 [26]. Эпидемиология ФАС/ФАСН в нашей стране не изучена. Ни в одной стране нет стандартной системы учета по диагностике ФАС и ФАСН из-за различия применяемых методик исследования.
Биохимическое и патоморфологическое воздействие алкоголя на плод
В организме плода алкоголь быстро проникает через плаценту и гематоэнцефалический барьер, накапливается в амниотической жидкости, долго циркулирует в крови и тканях плода [27–29].
Токсическое действие алкоголя проявляется [30] торможением белкового синтеза и нарушением митоза клеток, что увеличивает риск проявления генных мутаций; задержкой клеточной миграции (в результате нарушается миграция нейронов из зародышевого слоя и развивается функциональная недостаточность центральной нервной системы); внутриутробной гипоксией и ишемией, снижением церебрального метаболизма кислорода и глюкозы, подавлением дыхания и биоэлектрической активности мозга; нарушением пролиферации нейронов из-за антагонизма к рецепторам NMDA; цитотоксическим эффектом на формирующиеся ткани плода, что вызывает гибель плода или развитие пороков органов и систем.
При биохимическом обследовании мозга новорожденных крысят от алкозависимых самок выявлены нарушения энергетического обмена, что вызывает развитие митохондриальной дисфункции в головном мозге новорожденных крысят, угнетение активности митохондриальной креатинфосфокиназы (м‐КФК) и малатдегидрогеназы (МДГ), угнетение АТФазной активности, что свидетельствует о нарушении основных функций митохондрий – продукции и транспорта энергии [30].
Научные данные о роли окислительного стресса в патологии беременности свидетельствуют о его важной патогенетической значимости [31–33]. Употребление (по данным анкетирования) даже малых доз алкоголя беременными приводит к дисбалансу в системе «перекисное окисление липидов – антиоксидантная защита» как у женщин, так и у новорожденных [32]. Следует отметить, что до настоящего времени зависимость метаболических стрессов от уровня лабораторно подтвержденных доз принимаемого алкоголя и никотина беременными и влияние этого на формирование пороков развития плода у женщин не изучено.
Фенотипические изменения мозгового и лицевого черепа, морфологические изменения ткани мозга
При диагностике ФАС прежде всего обязательно документируются три лицевых отклонения: почти невидимая верхняя губа, небольшой разрез глаз, гладкий желобок между носом и верхней губой. У детей с ФАС удлиненное и асимметричное лицо, низкий лоб, монгольское веко, глубоко расположенные ушные раковины, уплощенный затылок, маленький седловидный нос, расщелина неба, неправильный рост зубов. Часто встречается косоглазие [34, 35]; размер головы, общий объем мозга и отдельные структуры (таламус и базальные ганглии) [36, 37] меньше нормы. Отмечаются нарушения речи, внимания, плохая память [38–41].
По утверждению Bariselli S. et al., у детей с ФАСН при взрослении количество клеток коры может не меняться, но изменяются их морфология и распределение [42]. В гиппокампе наблюдаются долгосрочные нарушения нейрогенного процесса, уменьшается объем зубчатой борозды; выявляются нарушения пролиферативной активности, миграции нейронов и глиобластов, что вызывает изменение числа нейронов в лимбической системе [43]. В мозжечке уменьшается число клеток Пуркинье. Нередко встречается полное или частичное отсутствие мозолистого тела, уменьшается его толщина, изменяется форма [44].
Нарушение психики, поведенческие, неврологические нарушения
У детей, родившихся с признаками ФАС, в первые дни после рождения наблюдаются в 80–88% дефекты развития центральной нервной системы: мышечный гипер/гипотонус, зрительно-моторная дискоординация, гипервозбудимость (двигательное беспокойство, тремор, нарушение сна, беспричинный плач и т.д.), гидроцефалия [45, 46]. Физически дети развиваются медленнее сверстников. В первый год они отстают примерно на 40%. В дальнейшем возникают медицинские, образовательные, поведенческие, социальные проблемы. Такие дети имеют трудности в обучении и запоминании; умении удерживать внимание; общении и социализации и т.д.
ФАС у детей характеризуется врожденными пороками сердца, печени, почек, нарушением развития скелета и другими аномалиями. Отмечаются также нарушения слуха и зрения, снижаются функции иммунной системы [46].
Не у всех детей, подвергшихся внутриутробному воздействию алкоголя, выявляется ФАС, однако у многих из них могут наблюдаться отдельные его проявления или менее выраженные нарушения. Дети с ФАС часто нуждаются в обучении в специализированных школах, где они смогут реализовать свой потенциал; ребенка будут обучать тем действиям, которые он может усваивать.
Роль медицинских работников в просвещении молодежи о факторах риска развития фетального алкогольного синдрома
Исследования, проведенные в разных странах Всемирной организацией здравоохранения, выявили, что даже несколько бесед врача с женщинами детородного возраста о вреде алкоголя способствуют уменьшению употребления ими спиртного [47, 48]. Для предотвращения ФАС среди детей необходимы привлечение государственной политики, развитие просвещения на системном уровне, национальные информационные программы, а также профилактические меры (в частности, скрининг на употребление алкоголя матерями во время беременности). На сегодняшний день существует несколько опросников для скрининга: ТОСО (T-ACE), ТОПАС (TWEAK) и АУДИТ (AUDIT).
Необходимо обучать врачей методам опроса и способам краткосрочного вмешательства, которые помогут в донесении информации женщинам репродуктивного возраста о недопустимости употребления любых спиртных напитков и пива при планировании беременности и во время беременности с тем, чтобы предотвратить возникновение у новорожденных таких заболеваний, как ФАС и ФАСН [49, 50].
Заключение
Дети, рожденные с ФАС, нуждаются в постоянном наблюдении кардиологов, неврологов, психологов, логопедов, социальных педагогов и социальных работников. Даже если у ребенка нет внешних признаков ФАС, нарушения проявляются в умственном и психическом развитии. При ФАС наблюдается увеличение частоты различных заболеваний, в частности, рахита, дерматита, анемии.
ФАС является необратимым состоянием, при котором излечение невозможно. Единственный способ избежать пороков и аномалий развития у ребенка – полностью отказаться от употребления алкоголя при планировании и во время беременности.
Опросники позволяют установить принадлежность женщин к группе риска, а затем использовать соответствующие методы консультирования для уменьшения или прекращения употребления алкоголя до зачатия. Скрининг может быть осуществлен с помощью опросников и при определении биомаркеров этанола в крови.
Крайне важными для предотвращения ФАС и ФАСН являются распространение современной информации и передача знаний врачами, психологами, социальными педагогами и социальными работниками беременным и женщинам репродуктивного возраста о том, какой непоправимый вред наносит ребенку употребление ими алкоголя.
Необходимо привлечь внимание общества к проблеме ФАС, пропагандировать здоровый образ жизни, воспитывать культуру потребления алкоголя, так как повсеместная доступность спиртных напитков и отсутствие самодисциплины приводят к пагубным последствиям.
Таким образом, проблема ФАС и ФАСН актуальна и требует тщательного дальнейшего изучения.
- Каткова И.П., Рыбальченко С.И. Бремя алкогольной смертности в России и ряде европейских стран. Социально-экономическое развитие государств Евразии и других зарубежных стран. Проблемы современной экономики. 2018; 3: 206-12. [Katkova I.P., Rybalchenko S.I. The burden of alcohol mortality in Russia and a number of European countries. Socio-economic development of the states of Eurasia and other foreign countries. Problems of Moderin Economics. 2018; (3): 206-12. (in Russian)].
- World Health Organization. Global status report on alcohol and health. World Health Organization; 2018. Available at: https://www.who.int/publications/i/item/9789241565639 13.10.2022.
- Popova S., Lange S., Probst C., Gmel G., Rehm J. Estimation of national, regional, and global prevalence of alcohol use during pregnancy and fetal alcohol syndrome: a systematic review and meta-analysis. Lancet Glob. Health. 2017; 5(3): 290-9. https://dx.doi.org/1016/S2214-109X(17)30021-9.
- Popova S., Lange S., Temple V., Poznyak V., Chudley A.E., Burd L. et al. Profile of mothers of children with fetal alcohol spectrum disorder: a population-based study in Canada. Int. J. Environ. Res. Public Health. 2020; 17(21): 7986.https://dx.doi.org/10.3390/ijerph17217986.
- Марянян А.Ю., Калькова А.Н. Современный взгляд на тератогенное влияние алкоголя при беременности. Возможные меры профилактики. Акушерство, гинекология и репродукция. 2022; 16(1): 48-57. [Marianian A.Yu., Kalkova A.N. A modern view on the teratogenic effect of alcohol during pregnancy. Possible preventive measures. Obstetrics, Gynecology and Reproduction. 2022; 16(1): 48-57. (in Russian)].https://dx.doi.org/10.17749/2313-7347/ob.gyn.rep.2021.254.
- Addila A.E., Bisetegn T.A., Gete Y.K., Mengistu M.Y., Beyene G.M. Alcohol consumption and its associated factors among pregnant women in Sub-Saharan Africa: a systematic review and meta-analysis' as given in the submission system. Subst. Abuse Treat. Prev. Policy. 2020; 15(1): 29. https://dx.doi.org/10.1186/s13011-020-00269-3.
- Hanson J.D., Oziel K., Sarche M., MacLehose R.F., Rosenman R., Buchwald D. A culturally tailored intervention to reduce risk of alcohol-exposed pregnancies in American Indian communities: Rationale, design, and methods. Contemp. Clin. Trials. 2021; 104: 106351. https://dx.doi.org/10.1016/j.cct.2021.106351.
- Treskina N.A., Postoev V.A., Usynina A.A., Grjibovski A.M., Odland J.Ø. Secular trends of socio-demographic and lifestyle characteristics among delivering women in Arctic Russia, 1973-2017. Int. Circumpolar. Health. 2023; 82: 2161131. https://dx.doi.org/1080/22423982.2022.2161131.
- Lemoine P., Harousseau H., Borteyru J.P., Menuet J.C. Les enfants de parents alcooliques: anomalies observees a propos de 127 cas. Ouest Medicale. 1968; 21(2): 476-82.
- Jones K.L., Smith D.W. Recognition of the fetal alcohol syndrome in early infancy. Lancet. 1973; 2: 999-1001.
- Calhoun F., Warren K. Fetal alcohol syndrome: historical perspectives. Neurosci. Biobehav. Rev. 2007; 31(2): 168-71. https://doi.org/10.1016/j.neubiorev.2006.06.023.
- Ikehara S., Kimura T., Kakigano A., Sato T., Iso H. Association between maternal alcoholconsumption during pregnancy and risk of preterm delivery: the Japan Environment and Children’s Study. BJOG. 2019; 126(12): 1448-55.https://dx.doi.org/10.1111/1471-0528.15899.
- Brown J.M., Bland R., Jonsson E., Greenshaw A.J. The standardization of diagnostic criteria for fetal alcohol spectrum disorder (FASD): implications for research, clinical practice and population health. Can. J. Psychiatry. 2019; 64(3): 169-76. https://dx.doi.org/10.1177/0706743718777398.
- Бюллетень Всемирной организации здравоохранения. 2011; 89(6): 398-9. [Bulletin of World Health Organization. 2011; 89(6): 398-9. (in Russian)]. https://dx.doi.org/10.2471/BLT.11.020611.
- Малахова Ж.Л., Шилко В.И., Бубнов А.А. Фетальный алкогольный синдром у детей раннего возраста. М.; 2012. 164с. [Malakhova Zh.L., Shilko V.I., Bubnov A.A. Fetal alcohol syndrome in children of early age. Moscow; 2012. 164p. (in Russian)].
- Вalashova T.N.; Prevent FAS Research Group. Developing education-al materials for prevention of FASD in Russia. CDC Grantees. Meeting 14-15 August, 2008. Atlanta; 2008.
- Murawski N.J., Moore E.M., Thomas J.D., Riley E.P. Advances in diagnosis and treatment of fetal alcohol spectrum disorders: from animal models to human studies. Alcohol Res. 2015; 37(1): 97-108.
- Astley S.J., Clarren S.K. Diagnostic guide to FAS and related condi-tions: the 4-digit diagnostic code. 1st ed. Monograph. Seattle: Univer-sity of Washington Publication Services; 1997. 138p.
- Bertrand J. National task force on FAS/FAE fetal alcohol syndrome: guidelines for referral and diagnosis. Monograph. Atlanta GA: Centers for Disease Control and Prevention; 2004. 179p.
- Hoyme H.E., May P.A., Kalberg W.O.., Kodituwakku P., Gossage J.P., Trujillo P.M. et al. A practical clinical approach to diagnosis of fetal alcohol spectrum disorders: clarification of the 1996 institute of medi-cine criteria. Pediatrics. 2005; 115(1): 39-47. https://dx.doi.org/10.1542/peds.2004-0259.
- Chudley A.E., Conry J., Cook J.L., Loock C., Rosales T., LeBlanc N. Fetal alcohol spectrum disorder: Canadian guidelines for diagnosis. CMAJ. 2005; 172(5,Suppl.): S1-S21. https://dx.doi.org/10.1503/cmaj.1040302.
- Hur Y.M., Choi .J, Park S., Oh S.S., Kim Y.J. Prenatal maternal alcohol exposure: diagnosis and prevention of fetal alcohol syndrome. Obstet. Gynecol. Sci. 2022; 65(5): 385-94. https://dx.doi.org/10.5468/ogs.22123.
- Colom J., Segura-García L., Bastons-Compta A., Astals M., Andreu-Fernandez V., Barcons N. et al. Prevalence of fetal alcohol spectrum disorders (FASD) among children adopted from eastern european countries: Russia and Ukraine. Int. J. Environ. Res. Public Health. 2021; 18(4): 1388. https://dx.doi.org/10.3390/ijerph18041388.
- May P.A., Fiorentino D., Phillip Gossage J., Kalberg W.O., Eugene Hoyme H., Robinson L.K. et al. Epidemiology of FASD in a province in Italy: Prevalence and characteristics of children in a random sample of schools. Alcohol. Clin. Exp. Res. 2006; 30(9): 1562-75. https://dx.doi.org/10.1111/j.1530-0277.2006.00188.x.
- May P.A., de Vries M.M., Marais A.S., Kalberg W.O., Buckley D., Hasken J.M. et al. The prevalence of fetal alcohol spectrum disorders in rural communities in South Africa: A third regional sample of child characteristics and maternal risk factors. Alcohol. Clin. Exp. Res. 2022; 46(10): 1819-36.https://dx.doi.org/10.1111/acer.14922.
- Murakami K., Obara T., Ishikuro M., Ueno F. Noda A., Kuriyam Sh. et al. Associations of education and work statuswith alcohol use and cessation amongpregnant women in Japan: The Tohoku Medical Megabank Project Birth and Three-Generation Cohort Study. BMC Public Health. 2021; 21(1): 1400. https://dx.doi.org/10.1186/s12889-021-11461-w.
- Robert M., Carceller A., Domken V., Ramos F., Dobrescu O., Simard M. et al. Physical and neurodevelopmental evaluation of children adopted from Eastern Europe. Can. J. Clin. Pharmacol. 2009; 16(3):e432-40.
- Skagerstrуm J., Chang G., Nilsen P. Predictors of drinking during pregnancy: a systematic review. J. Womens Health. 2011; 20(6): 901-13.https://dx.doi.org/10.1089/jwh.2010.2216.
- Марянян А.Ю., Калькова А.Н., Акудович Н.В. Влияние алкоголя на биоэлементный статус беременных женщин, употребляющих алкоголь в пренатальном периоде. Акушерство и гинекология. 2021; 10: 21-30. [Marianian A.Yu., Kalkova A.N., Akudovich N.V. Influence of alcohol consumption on the bioelement status of pregnant women in the prenatal period. Obstetrics and Gynecology. 2021; (10): 21-30. (in Russian)].https://dx.doi.org/10.18565/aig.2021.10.21-30.
- Беленичев И.Ф., Соколик Е.П., Егоров А.Н. Фармакологическая модуляция компенсаторных механизмов энергетического метаболизма в головном мозге пренатально алкоголизированных животных. Вестник новых медицинских технологий. 2014; 3: 16. [Belenichev I.F., Sokolik E.P., Egorov A.N. Pharmacological modulation of compensatory mechanisms of energy metabolism in the brain of prenatally alcoholic animals. Bulletin of New Medical Technologies. 2014; (3): 16. (in Russian)].
- Darenskaya M.A., Kolesnikov S.I., Rychkova L.R., Grebenkina L.A., Kolesnikova L.I. Oxidative stress and antioxidant defense parameters in different diseases: ethnic aspects. Free Radic. Biol. Med. 2018; 120(Suppl. 1): S60.
- Колесникова Л.И., Даренская М.А., Колесников С.И. Свободнорадикальное окисление: взгляд патофизиолога. Бюллетень сибирской медицины. 2017; 16(4): 16-29. [Kolesnikova L.I., Darenskaya M.A., Kolesnikov S.I. Free radical oxidation: A view of a pathophysiologist. Bulletin of Siberian Medicine. 2017; 16(4): 16-29. (in Rus-sian)]. https://dx.doi.org/10.20538/1682-0363-2017-4-16-29.
- Marianian A., Atalyan A., Bohora S., Darenskaya M., Grebenkina L., Kolesnikova L. et al. The effect of low alcohol consumption during pregnancy on the lipid peroxidation-antioxidant defense system of women, their alcohol-exposed infants, and growth, health, and developmental outcomes. Birth Defects Res. 2019; 112(1): 40-53. https://dx.doi.org/10.1002/bdr2.1582.
- Subramoney S., Eastman E., Adnams C., Stein D.J., Donald K.A. The early developmental outcomes of prenatal alcohol exposure: a review. Front. Neurol. 2018; 9: 1108. https://dx.doi.org/10.3389/fneur.2018.01108.
- Garrison L., Morley S., Chambers C.D., Bakhireva L.N. Forty Years of Assessing Neurodevelopmental and Behavioral Effects of Prenatal Alcohol Exposure in Infants: What Have We Learned? Alcohol. Clin. Exp. Res. 2019; 43(8): 1632-42. https://dx.doi.org/10.1111/acer.14127.
- Колпаков Я.В., Ялтонская А.В., Ялтонский В.М., Абросимов И.Н. Методология диагностики фетального алкогольного спектра нарушений у детей младшего школьного возраста в России. Вопросы наркологии. 2017; 4-5: 153-163. [Kolpakov Ya.V., Yaltonskaya A.V., Yaltonsky V.M., Abrosimov I.N. Methodology for diagnosing fetal alcohol spectrum disorders in children of primary school age in Russia. Questions of Narcology. 2017; 4-5: 153-63. (in Russian)].
- Hoyme H.E., Kalberg W.O., Elliott A.J., Blankenship J., Buckley D., Marais A.S. et al. Updated clinical guidelines for diagnosing fetal alcohol spectrum disorders. Pediatrics. 2016; 138(2): e20154256. https://dx.doi.org/10.1542/peds.2015-4256.
- Uban K.A., Kan E., Wozniak J.R., Mattson S.N., Coles C.D., Sowell E.R. The relationship between socioeconomic status and brain volume in children and adolescents with prenatal alcohol exposure. Front. Hum. Neurosci. 2020; 14: 85. https://dx.doi.org/10.3389/fnhum.2020.00085.
- Subramoney S., Joshi S.H., Wedderburn C.J., Lee D., Roos A., Woods R.P. et al. The impact of prenatal alcohol exposure on gray matter volume and cortical surface area of 2 to 3-year-old children in a South African birth cohort. Alcohol. Clin. Exp. Res. 2022; 46(7): 1233-47. https://dx.doi.org/10.1111/acer.14873.
- Poth L.D., Love T., Mattson S.N. Profiles of language and communication abilities in adolescents with fetal alcohol spectrum disorders. J. Int. Neuropsychol. Soc. 2022; Nov.3: 1-10. https://dx.doi.org/10.1017/S1355617722000789.
- Gautam P., Lebel C., Narr K.L., Mattson S.N., May P.A., Adnams C.M. et al. Volume changes and brain-behavior relationships in white matter and subcortical gray matter in children with prenatal alcohol exposure. Hum. Brain Mapp. 2015; 36(6): 2318-29. https://dx.doi.org/10.1002/hbm.22772.
- Bariselli S., Lovinger D.M. Corticostriatal circuit models of cognitive impairments induced by fetal exposure to alcohol. Biol. Psychiatry. 2021; 90(8): 516-28. https://dx.doi.org/10.1016/j.biopsych.2021.05.014.
- Gil-Mohapel J., Boehme F., Patten A., Cox A., Kainer L., Giles E. et al. Altered adult hippocampal neuronal maturation in a rat model of fetal alcohol syndrome. Brain Res. 2011; 1384: 29-41. https://dx.doi.org/10.1016/j.brainres.2011.01.116. 21.
- Delatour L.C., Pamela W.L. Yeh, Yeh H.H. Prenatal exposure to ethanol alters synaptic activity in layer V/VI pyramidal neurons of the somatosensory cortex. Cerebral Cortex. 2020; 30(3): 1735-51. https://dx.doi.org/10.1093/cercor/bhz199.
- Wozniak J.R., Mueller B.A., Muetzel R.L., Bell C.J., Hoecker H.L., Nelson M.L. et al. Inter-hemispheric functional connectivity disruption in children with prenatal alcohol exposure. Alcohol. Clin. Exp. Res. 2011; 35(5): 849-61.https://dx.doi.org/10.1111/j.1530-0277.2010.01415.x.
- Cook J.L., Green C.R., Lilley C.M., Anderson S.M., Baldwin M.E., Chudley A.E. Fetal alcohol spectrum disorder: Aguideline for diagnosis across the lifespan. CMAJ. 2016; 188(3): 191-7. https://dx.doi.org/10.1503/cmaj.141593.
- Фонд Организации Объединенных Наций в области народонаселения (ЮНФПА). Программа действий международной конфедерации по народонаселению и развитию. Принятая на Международной конференции по народонаселению и развитию. Каир, 5-13 сентября 1994 г. Доступно по: https://www.unfpa.org/sites/default/files/event-pdf/icpd_rus.pdf [United Nations Population Fund (UNFPA). Programme of Action of the International Conference on Population and Development. Adopted by the International Conference on Population and Development. Cairo, 5-13 September 1994. Available at: https://www.unfpa.org/sites/default/files/event-pdf/icpd_rus.pdf (in Russian)].
- Marianian A.Yu., Molchanova E.V. Social and economic effect of comprehensive prevention of fetal alcohol syndrome and fetal alcohol spectrum disorders in children: a review. J. Pharmaceutical Res. Int. 2020; 32(23): 115-23.https://dx.doi.org/10.9734/jpri/2020/v32i2330798.
- Burina E.A., Kulieva A.K., Marianian A.Y. The risk of fetal alcohol syndrome in pregnant women and women planning pregnancy. Alcoholism: Clin. Exp. Res. 2018; 42(6): 75. https://dx.doi.org/10.1111/acer.13833.
- Бурина Е.А., Марянян А.Ю. Психологические аспекты профилак-тики фетального алкогольного синдрома у беременных женщин репродуктивного возраста. Acta Biomedica Scientifica. 2018; 3(3):149-54. [Burina E.A., Marianian A.Yu. Psychological aspects of fetal alcohol syndrome prevention in pregnant women of childbearing age. Acta Biomedica Scientifica. 2018; 3(3): 149-54. (in Russian). https://dx.doi.org/10.29413/ABS.2018-3.3.23.
- Шилко В.И., Малахова Ж.Л., Бубнов А.А., Сергеева Л.М. Фетальный алкогольный спектр нарушений среди воспитанников домов ребенка. ВолГМУ. 2010; 4: 108-11. [Shilko V.I., Malakhova J.L., Bubnov A.A., Sergeeva L.M. Fetal alcohol syndrome in orphanage children. VolGMU. 2010; (4): 108-11. (in Russian)].
Received 18.11.2022
Accepted 27.04.2023
Anait Yu. Marianian, Dr. Med. Sci., Head of the Laboratory of Socially Important Problems of Reproductology, Leading Researcher, Scientific Center of Family Health Problems and Human Reproduction; Associate Professor at the Department of Obstetrics and Gynecology, ISMAPGE – Branch of the RMACPE, Ministry of Health of Russia, +7(3952)20-76-36, +7(914)014-70-65,
anait_24@mail.ru,
iphr@sbamsr.irk.ru, https://orcid.org/0000-0002-9544-2172, 664003, Russia, Irkutsk, Timiryazev str., 16.
Anastasia O. Anisimova, clinical intern and laboratory researcher at the Laboratory of Socially Important Problems of Reproductology, Scientific Center of Family Health Problems and Human Reproduction, +7(950)126-98-60,
mozolewaao@gmail.com, https://orcid.org/0000-0003-2067-4224, 664003, Russia, Irkutsk, Timiryazev str., 16.
Anastasia N. Kalkova, graduate student and research assistant at the Laboratory of Socially Important Problems of Reproductology, Scientific Center of Family Health Problems and Human Reproduction, +7(902)576-00-19,
Kalkova_Nastya@mail.ru, https://orcid.org/0000-0002-7626-020X, 664003, Russia, Irkutsk, Timiryazev str., 16.
Maria A. Rashidova, PhD, Researcher at the Laboratory of Physiology and Pathology of the Endocrine System, Scientific Center of Family Health Problems and Human Reproduction, +7(3952)20-76-36, 20-73-67,
rashidovama@mail.ru, https://orcid.org/0000-0003-4730-5154, 664003, Russia, Irkutsk, Timiryazev str., 16.
Lyubov V. Rychkova, Professor, Dr. Med. Sci., Corresponding Member of the Russian Academy of Sciences, Director, Scientific Center of Family Health Problems and
Human Reproduction, +7(3952)20-76-36, 20-73-67,
iphr@sbamsr.irk.ru, https://orcid.org/0000-0002-0117-2563, 664003, Russia, Irkutsk, Timiryazev str., 16.
Artyom E. Muradyan, 6th year student of the Faculty of Pediatrics, Pirogov Russian National Research Medical University, Ministry of Health of Russia,
+7(495)434-05-43, +7(919)724-54-79, don.muradian@yandex,
rsmu@rsmu.ru, https://orcid.org/0000-0001-5350-0453, 117997, Russia, Moscow, Ostrovityanova str., 1.
Corresponding author: Anastasia O. Anisimova,
mozolewaao@gmail.com



